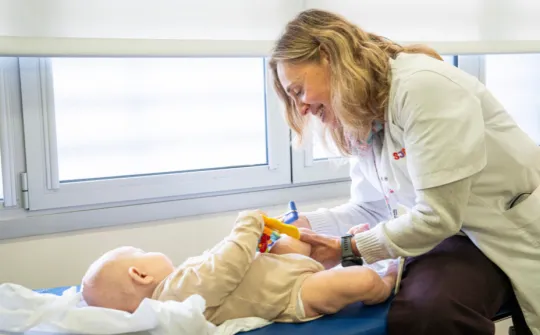
"In the near future we'll be able to bioprint 3D compatible tissues and organs to implant in patients"
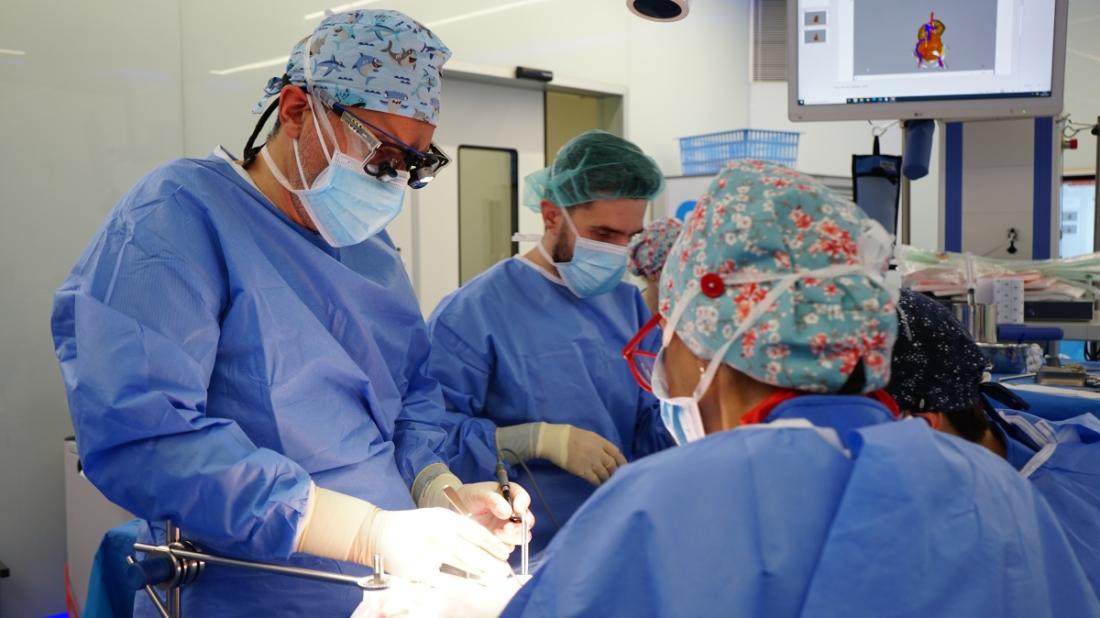
Dr. Lucas Krauel explains how paediatric oncological surgery has evolved at SJD Barcelona Children's Hospital since the first 3D reproduction in 2014.
Dr. Lucas Krauel explains how paediatric oncological surgery has evolved at SJD Barcelona Children's Hospital since the first 3D reproduction in 2014.
SJD Barcelona Children's Hospital hosts the annual International Congress on Paediatric Oncological Surgery (IPSO) led by Dr. Lucas Krauel, which provides answers to some of the key questions on this subject. The IPSO Pediatric Surgical Oncology Educational Day: Ped Surg Onc Team Building coordinated by the Sant Joan de Déu training team takes place in the month of September.
What are the objectives of the paediatric oncology surgical training and what do you expect participants to take away from it?
The main objective of this training event is to highlight the importance of teamwork. Under this year’s motto, “Team Building”, we’ll hear from everyone involved in oncological surgery: surgeons, anaesthesiologists, the radiologists who help to determine the exact location for biopsies, experts in 3D models for surgical planning, specialists in nuclear medicine, etc. The aim is to improve the prognosis of paediatric patients, reduce the sequelae of the disease and prolong the life expectancy of children.
World-renowned surgeons from American hospitals will be attending, such as Dr. LaQuaglia, one of the world's foremost surgical oncologists from the Memorial Sloan Kettering Cancer Center in New York, who will talk about complex approaches in paediatric surgical oncology. Oncology experts from other hospitals such as Boston Children's Hospital and hospitals in Brazil, Argentina and Mexico, among others, will also participate. At the European level, professionals from hospitals such as the Hospital Necker in France or the Prinses Maxima Centrum in the Netherlands will also attend.
What role do you think simulation can play as a training and refresher tool for paediatric surgeons?
Each tumour and each patient is different, so each case needs to be carefully studied and planned in a personalised way. In this respect, simulation is very helpful. The more prepared we are, the better the surgery will go. We are currently working with 3D tumour reproduction and virtual reality to analyse tumours, practise surgical procedures and anticipate situations that one can encounter during an operation.
SJD Barcelona Children's Hospital is a pioneer and world leader in 3D tumour reproduction, which is used to plan complex operations. The first 3D reproduction took place in 2014, and since then, the hospital’s 3D Simulation and Planning Unit has grown stronger and advances have been made in the use of materials. The aim is to ensure that what is 3D printed is as close to reality as possible. For example, we’ve created tissue that’s very close to the real thing in reproductions of organs such as the liver.
We also have virtual reality glasses that allow us to visualise the organ we’re going to operate on in an immersive way, we can rotate it, see it in 360º in a totally immersive way in order to thoroughly understand the tumour and the anatomical area to be treated so that we can plan the operation accordingly.
We’re also working on an augmented reality project which will allow us to see the tumour in the real environment, consult the image and manipulate it.
What are the challenges facing cancer surgery in the coming years?
The greatest challenge is to achieve complete resections of the most complex tumours. Unfortunately, there are still situations where surgery is not a viable option. In this regard, in the future the simulation would be projected in the operating theatre, in real time, as we're operating, and would alert us to possible problems that we may encounter, this will help us to improve outcomes.
In the near future we’ll also be able to 3D print compatible tissues and organs to implant in patients.
Another challenge concerns the advancement of robotic surgery to help us make operations just as effective but less invasive.
Can you tell us about any other advances in the works?
Many international research groups are working on new drug delivery systems to better reach the tumour and have fewer side effects. In this area, SJD Barcelona Children's Hospital collaborates with Cebiotex, a spin-off sponsored by the Hospital and the Universitat Politècnica de Catalunya (UPC) for the development of biodegradable nanofibres filled with chemotherapy. These nanofibres are applied to the operated area to control resection margins and residual microscopic disease that may remain after surgical excision. The controlled release of the chemotherapeutic agent is possible thanks to the nanostructure. Trials are currently underway in adults, and once it works it will also be applied to paediatric cancer.