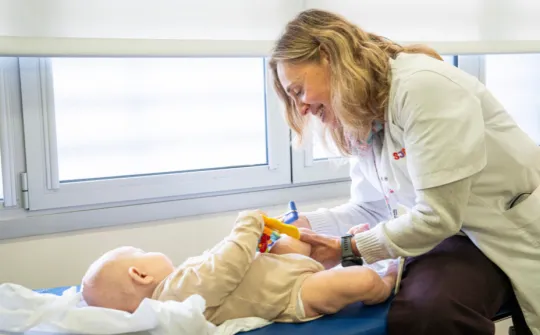
The SJD Barcelona Children's Hospital implements the "SJD at Home" programme, which is consolidating during the coronavirus pandemic.
“We needed to have more beds available in the Hospital for patients who really needed them, and we were also convinced that the boys and girls are better off at home”. This is the point of departure which Juan José García, head of the Pediatric Department of the SJD Barcelona Children's Hospital, identifies as the beginning of the Hospital's "SJD at Home" programme, a groundbreaking initiative in pediatric hospital care in Spain.
In spring 2019, the Hospital launched a pilot programme with 95 patients to evaluate the possibility of setting up home care in an initial group of children. The trial lasted three months and helped the Hospital to ascertain the type of profile of families who could participate in home hospitalisation in order to evaluate the initial findings. The programme, now consolidated, frees up between 6 and 12 beds a day in the center: "it is like having a ward outside the Hospital", says Juan José García.
Training the families, the key to the programme's success
About 90% of the patients who take part in this programme usually come from conventional hospitalisation, whereas the other 10% come directly from the Emergency department or Outpatient departments. The teams which look after them detect which families and patients are possible candidates for participating in the programme. The family is offered the chance of hospitalising the child at home, and, if they agree, a specialist nurse provides them with training, including the child if he or she is old enough, in carrying out the procedures and in giving the necessary care at home.
Remote monitoring is performed with the help of a remote monitoring kit comprised of several devices: a tablet for making video calls and for data input, as well as other devices such as an oximeter, scales or a thermometer. The remote monitoring equipment not only provides families with reassurance, it also enables the medical team to detect if something is not progressing correctly and to contact the family. For in situ monitoring, a team comprised of a pediatrician and a nurse makes home visits, generally on a daily basis.
The pediatrician who is in charge of the pediatric home hospitalisation programme, Astrid Batlle, explains that there are two main patient groups: those with respiratory conditions and those with some kind of infection. For the first group, families are trained to administer oxygen therapy and nebulisations at home and also how to recognise warning signs and respiratory distress. In the second group, children with infections, the parents are taught how to administer intravenous antibiotics, make sure that the line is properly in place, give the medication and also recognise warning signs. There are also many other types of patients, albeit fewer in number.
The results of the pilot test show great acceptance from families
The evaluation made by the Hospital and participants alike was very good. Most of the families polled (77%) said that the first home visit took place within less than 24 hours after home hospitalisation began. Virtually all of the respondents who had requested some type of help said that the response was very quick (91%), and over 90% of the families managed to measure the vital signs correctly with the tools provided.
Ninety-seven percent (97%) said that the workload involved in caring for the child was lower than they initially imagined and they were particularly appreciative of the way in which the pediatric and nursing team worked in coordination. All the respondents said that the duration of the home visit was sufficient. Moreover, most of the families polled concluded that they would repeat the experience if they could and rated the healthcare received as "excellent". Furthermore, in most of the cases it has not been necessary to re-admit the children to hospital and practically all of the patients who participated in the programme have been treated and discharged at home.
Consolidation during the coronavirus pandemic
In the state of emergency resulting from the COVID-19 pandemic, the pediatric home hospitalisation programme has continued to operate and also helped to provide healthcare to some of the patients affected, thus minimising the risk of contacts. A total of eleven patients with the SARS-CoV-2 virus (9 children and 2 adults) have been provided with home care and 57 home PCRs have been performed. This form of hospitalisation, together with remote care, are two of the tools that will enable the SJD Barcelona Children's Hospital to reduce the influx of patients and hospitalisations during the pandemic.
Since the programme was implemented on a permanent basis in 2019, a total of 366 patients were treated at home, with an average stay of 4.7 days. The fact that the patient is treated at home, as the pediatrician Astrid Batlle explains, is not only in keeping with the Charter of Rights of Children in Hospital, but also reduces the risk of infections from the clinical standpoint. Furthermore, patients and families who opt into the home hospitalisation programme must be proactive, and this programme equips them with tools to look after their own health, which in turn provides them with reassurance.
"It has been challenging for the team of professionals, since working in a hospital gives you a safe and controlled setting, whereas doing so outside calls for a great deal of flexibility", explains Batlle. The pediatrician concludes: "We are learning a great deal and we are detecting practices in the home which we think could be applied to the Hospital to improve the quality of life of hospitalised children. The programme stimulates a flow of ideas and information from home to ward and vice-versa".