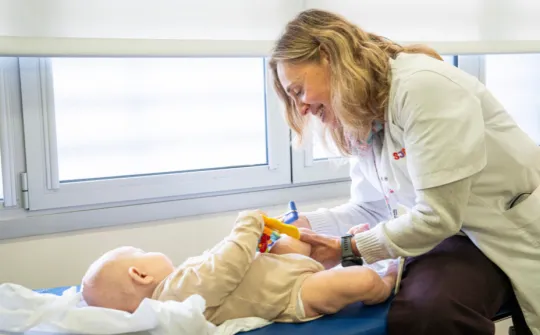
SJD Barcelona Children's Hospital consolidates the dental autotransplantation technique with the help of 3D printing
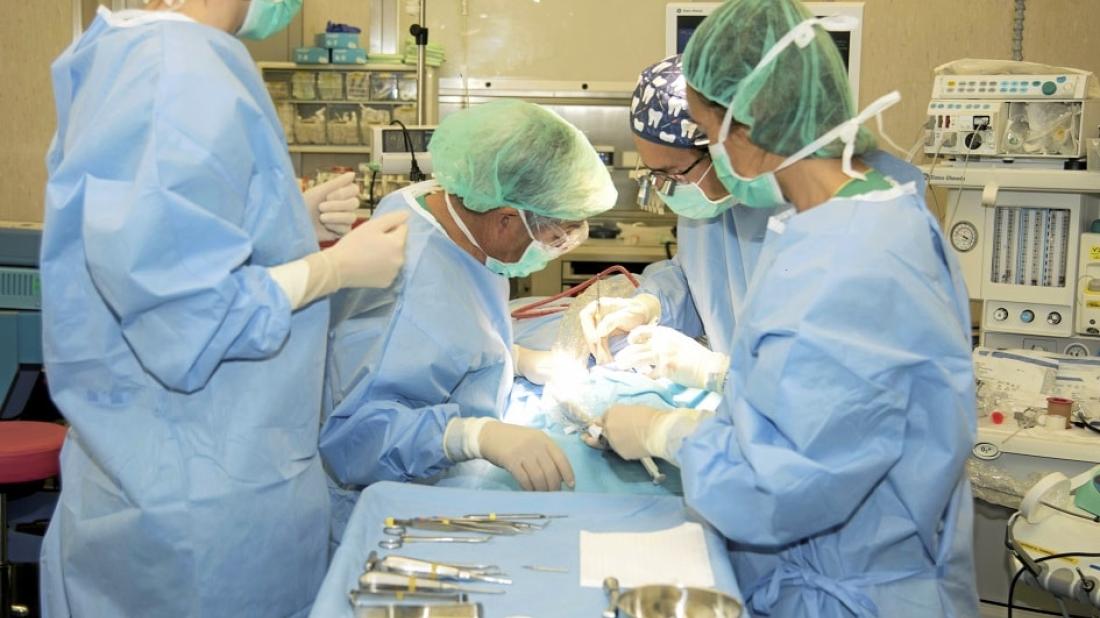
The 3D technology allows us to create a replica from resin to check the suitability of the transplanted tooth and improve the result.
Since 2018, the Dentistry and Orthodontics team at SJD Barcelona Children's Hospital has performed nine autotransplantations using this technique , which has already been performed on five patients this year. The consolidation of the department will serve to treat some minor dental diseases as well as cases that require the replacement of teeth that are damaged or in poor condition.
The first autotransplantation was performed on a 16-year-old patient who had started malposition (ectopic) treatment through an orthodontist. It was revealed that she had a milk tooth that had not fallen out, and so the permanent tooth, a mandibular premolar, had not been able to come through. The Dentistry team decided to remove the milk tooth to see if the premolar would come through on its own.
Six months later, on seeing that the patient did not progress as expected, outpatient surgery was performed for the orthodontic traction of the premolar. The aim was to allow the tooth to come through after this facilitating procedure, which is called an "eruption pathway". Once again, the patient's progress was not favourable. It was at this point that the possibility of extracting (removing) the blocked tooth was proposed, with an autotransplant of this tooth being performed after.
One of the difficulties of this type of intervention is ensuring that the premolar socket area is exact and that the recipient bed is appropriate. Another challenge is reducing the handling time of the tooth being transplanted during the surgery, in order to prevent the deterioration (necrosis) that occurs in the minutes after the tooth is extracted. In the past, these checks were performed using the tooth itself, an action that could damage the root during surgery and jeopardise the prognosis.
From 3D simulation to the operating room
To prevent damage to the root of the tooth, we opted for the use of 3D technology, which allowed us to plan the surgery and study the part of the jaw where the autoimplant would be carried out. This also allowed us to create a replica of the tooth using resin, which acted as a guide in the operating room.
Thanks to the resin piece reproduced using 3D techniques, we were able to check the fit of the replica in the space that had been created (the new presurgical alveolus) where the transplanted tooth would be placed. We were also able to perform various tests with this piece during the surgery, thereby reducing the risks of damaging the patient's tooth during the procedure.
The extracted natural tooth was kept submerged in physiological serum during the surgery and was only handled at the end, after the tests with the replica had been performed, in order to place it inside the dental alveolus. This avoided extra manoeuvres being added to the process, which could have damaged it. After the intervention, the autotransplanted premolar was stabilised with the help of the patient's orthodontist.
The use of 3D planning in cases of severe dental ectopia (rare or uncommon cases) allows us to reduce the surgery time and other additional costs of treatment. The 3D printing used by the surgeon creates the replica at a minimal cost. This technology has enabled us to reduce the intervention time and has helped us avoid having to fit the patient with an osseointegrated titanium implant and crown.