The 3D Unit consolidates the planning and simulation of complex surgery and serves all paediatric specialties.
Presentation
In 2013, SJD Barcelona Children's Hospital planned the first-ever complex oncological surgical procedure using three-dimensional printing for a paediatric patient. Since then, the number of surgical specialties using this technology to plan or guide surgery has multiplied.
Currently, ten surgical specialties at the hospital use this type of technique to treat our patients (Orthopaedics and Traumatology, Maxillofacial Surgery, general and thoracic Plastic Surgery, Dentistry and Orthodontics, Oncology, Foetal Medicine, Neurology, Otorhinolaryngology and Cardiology).
The 3D Unit, a pioneer in Spain, has since been consolidated and offers solutions to all Departments and Units that request planning or use new technologies to improve the performance and safety of surgeries and other procedures. This Unit has received a license from the Generalitat de Catalunya as custom manufacturer of medical devices, complying with quality and regulation standards. The unit has the license to manufacture custom-made sanitary products EU MDR 2017/745 granted by the Generalitat (with code FMP003CAT) under the international quality system ISO 13485:2016.
Mixed model and interdisciplinary study of cases
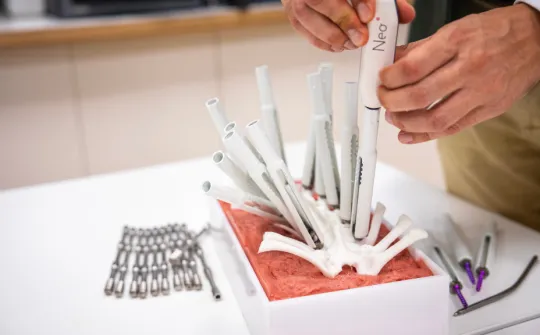
Professionals specialised in 3D planning and printing work under a mixed work model in a specific unit in the hospital itself. Here, virtual simulations and planning are done, anatomical models are printed and cutting and positioning guides are prepared. We also have an external team of professionals and suppliers who assist in more complex cases and custom implants. This model facilitates a more efficient and effective service to clinical teams and meets any planning challenges that may arise.
The cross-cutting, multidisciplinary team is coordinated by the Innovation Department and is made up of engineering experts, members of the Diagnostic Imaging Department, Surgery, the innovation, and biomedical engineering team, finance, and the Darwin Advanced Simulation Programme team. In addition, the hospital belongs to the Carlos III Health Institute (ISCIII) Biobanks and Biomodels Platform. The members of the unit study each case and assess the possibilities and clinical benefits to the patient of applying 3D techniques.
Clinical applications of 3D technology
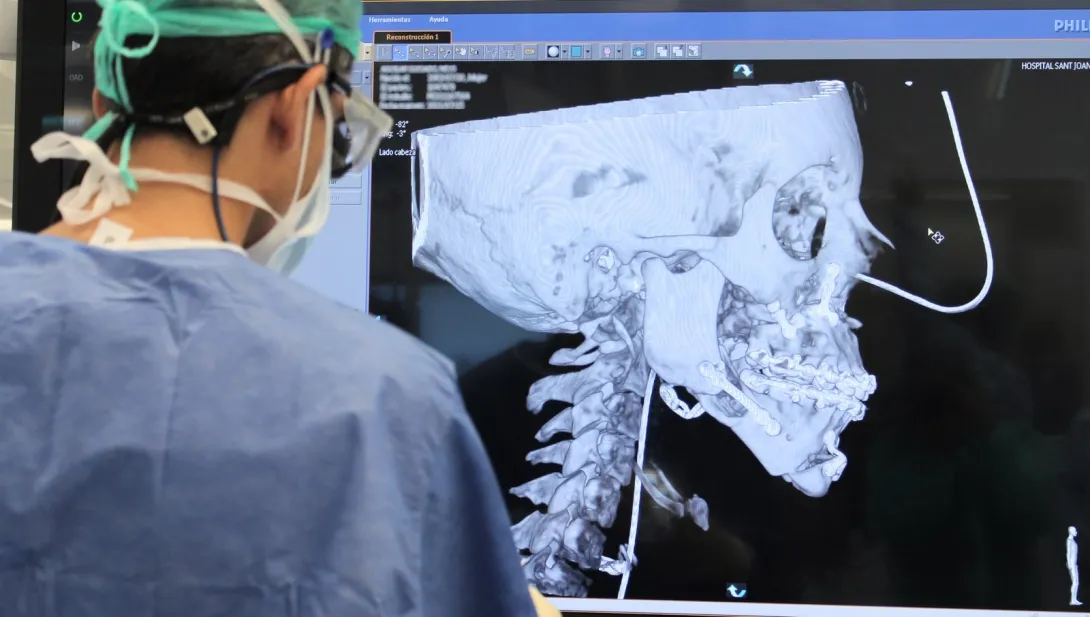
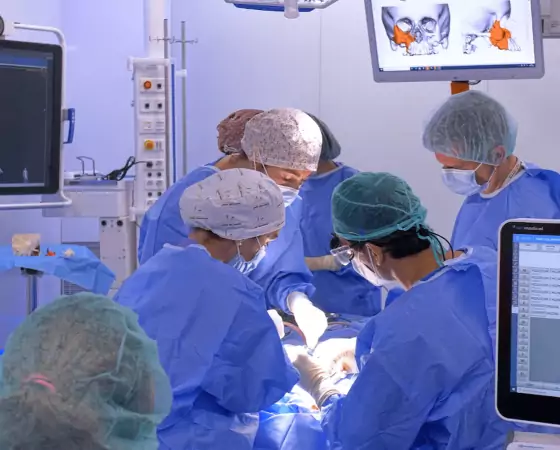
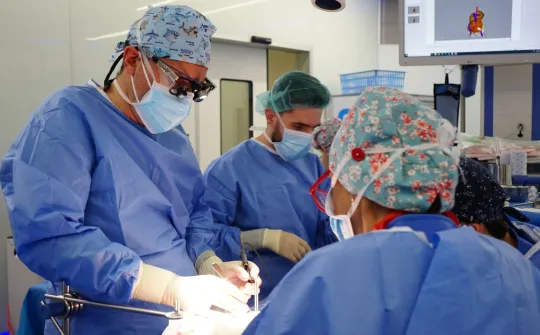
Planning (before and during surgery) allows the surgical approach to be simulated and tested, which is personalized and adapted to each individual patient. This achieves better outcomes and reduces surgery time.
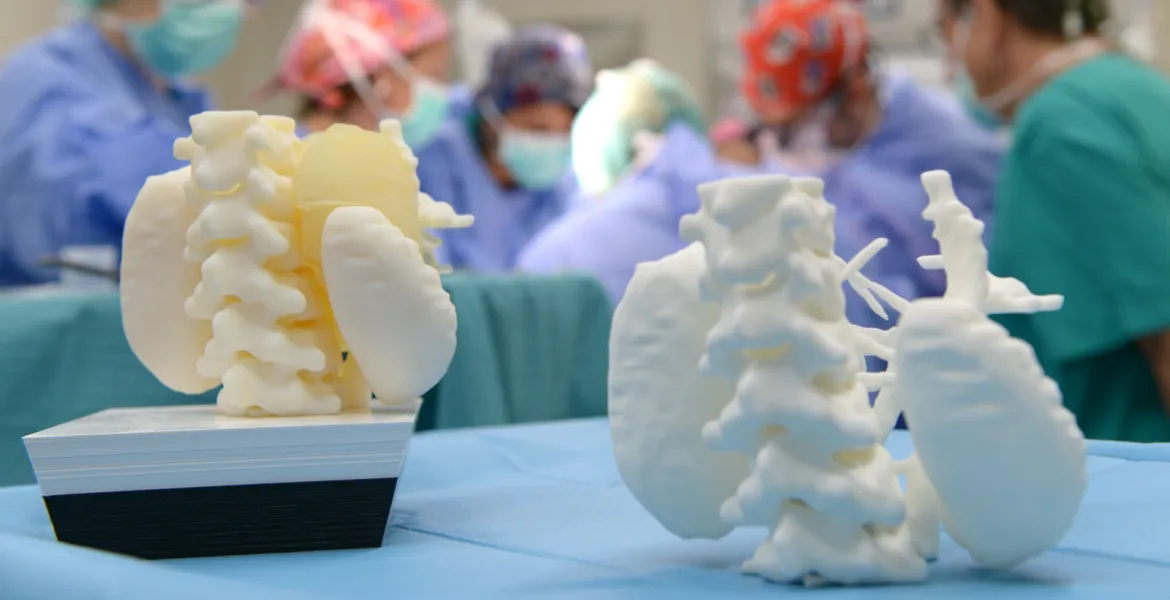
Life-size 3D modelling of tumours, organs and bones for use in medical training and research. The parts can be used by surgeons to prepare and explain surgery to families or to personalise osteosynthesis material.
In Maxillofacial Surgery and Orthopaedics and Traumatology, custom parts can be designed to guide the cuts and movements planned for surgery. This facilitates surgical precision and improves times and outcomes.
3D manufacturing makes it possible to offer solutions to children with mobility issues and amputations. Orthoses are normally used for rehabilitation and musculoskeletal correction.
3D models are used in teaching activities to simulate complex cases. Simulation and moulding techniques can be combined with 3D techniques to produce custom phantom models and simulators.
The different 3D printing techniques and materials allow generating prototypes with high precision and complexity requirements.
Advantages of 3D planning and printing
Process standardisation
A healthcare pathway has been established for all clinical departments in order to implement agile and optimized surgery planning processes.
Cumulative experience in complex cases enables techniques that can be repeated in the same disease to be applied and consolidated. For its part, standardization represents an improvement in process efficiency and offers tools available to surgeries such as physeal bridge resection, planning of surgeries for Pierre Robin syndrome, plastic surgery for cases of microtia, autologous tooth transplantation, and alveolar cleft correction.
Safety
Intervention trials allow a very high degree of precision and the anticipation of possible difficulties in the operating room. Thanks to the simulation and the previous practice of the surgeries, it is possible to reduce the anesthesia and ischemia time and the possible complications derived from the intervention, which translates into an improvement in patient safety.
For patients and families, this technology helps to better understand the surgical procedure to treat the disease.
Efficiency and efficacy
The planning reduces the time of surgical intervention, which allows a faster recovery of the patient and also a reduction of resources and costs. In cases of alveolar cleft reconstruction or reconstruction of the auricle, surgical time is reduced by up to 40%.
The precision in the approach makes it possible to obtain the planned result in practically all cases and reduce the rate of reoperation in patients.
Teaching and simulation
As a pioneer hospital unit in the use of 3D technology nationwide, it transmits knowledge within the framework of the Expert3D training program. The objective of this program is to provide health professionals with a theoretical and practical foundation in medical image post-processing, planned surgery, 3D printing and research imaging.
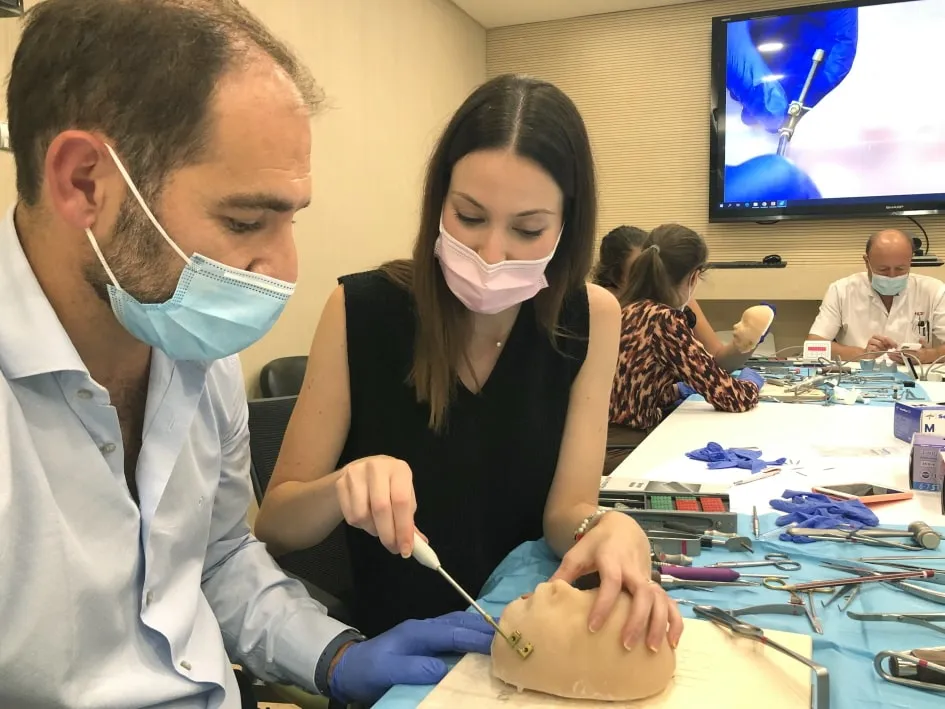
The 3D printed models are used in the teaching activity for the simulation of complex cases within the Darwin Advanced Simulation Program of the Sant Joan de Déu Hospital. The objective of the program is to improve the training of professionals and their work dynamics, in addition to facilitating clinical learning, giving medical professionals the opportunity to train in complex surgeries.
The 3D4H Unit has created different tailor-made simulators for facial malformations and complex pathologies from the newborn to adulthood, which have been used by professionals to practice before performing the intervention, to train residents and in specialized training courses.
Research
The 3D Unit participates in four European projects, including QuirofAM and Base3D (Fuse3D). During the pandemic, Sant Joan de Déu has also participated in the CAR3D project to combat COVID-19 through additive manufacturing. Recently, the "3DSurgHELP" project to study the use of virtual and augmented reality and 3D printing for surgical planning of complex surgeries has been financed by the Ministry of Science and Innovation and the Generalitat de Catalunya, with funds from the European Union NextGenerationEU.
3D unit outcomes
Yearly average of cases planned in 3D
Specialties using 3D planning
Reduced surgery time in certain cases
Publications since 2014
SJD Barcelona Children's Hospital 3D Unit team

Links of interest





ISCIII Biomedicine and Health Sciences R&D&I support platform. Biomodels - 3D Printing, Project Code PT20/00090, funded by the Instituto de Salud Carlos III, aid programme for ISCIII Biomedicine and Health Sciences R&D&I support platforms from Strategic Action in Health 2017-2020 and co-funded by the European Union through the European Regional Development Fund and the European Social Fund.