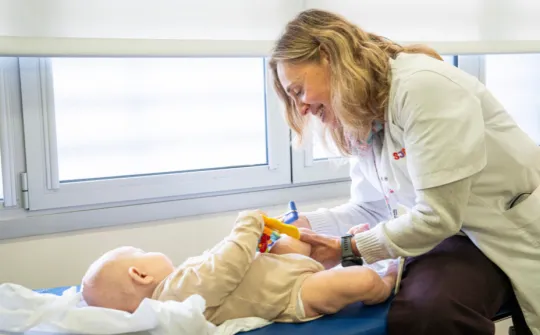
A team of neurosurgeons performs awake surgery on a 15 year old to excise the focus of her epilepsy

It is the first time SJD Barcelona Children’s Hospital has performed this complex operation on a conscious patient
- This type of surgery is performed in adults, but is not at all common in children and adolescents due to the collaboration required on the part of the patient.
- The adolescent suffered from very complex epilepsy, and the team in the Epilepsy Unit had to implant electrodes in her brain to diagnose the disease and define the area where the seizures were originating.
- The 15 year old patient had been suffering from epileptic seizures since she was three years old but has not had a single seizure since the operation.
75% of epilepsy cases appear in childhood. It is estimated that up to one in three do not respond to drugs. Some of these refractory cases can be treated surgically, and SJD Children’s Hospital Barcelona is one of the few reference centres in Spain for the surgical treatment of refractory epilepsy in children.
In very complex cases of epilepsy, neurosurgeons implant intracranial electrodes to monitor brain activity for one or two weeks for diagnostic purposes: to locate and define the area where the seizures are originating, its limits and its relationship to expressive areas, to determine whether it will be possible to remove it. This was the procedure used in the case of a 15 year old girl from Las Palmas in Gran Canaria who had suffered from epileptic seizures since she was three years old that were negatively affecting her day-to-day life. She was operated on by a team from SJD Barcelona Children’s Hospital that included neurologists, neuropaediatricians, neurosurgeons, neurophysiologists, neuroradiologists and neuropsychologists.
By implanting electrodes and monitoring the patient’s brain activity, it was possible to discover that the area where the seizures were originating was located in the left hemisphere of the brain and included the area that connects the occipital and temporal lobes, i.e. the area that connects the vision and language centres and is involved in reading. The surgeons decided that excising the area where the seizures were originating was a viable option, but decided to do it with the patient awake and reading in order to ensure this ability was not damaged. This type of procedure is performed in adults, but is not at all common in children and adolescents due to the collaboration required on the part of the patient.
Neurostimulation, monitoring and teamwork: the keys to the surgery’s success
The operation lasted six hours and the patient had to be prepared beforehand, by instructing her on the tasks she would have to perform in theatre during the three hours for which she would be awake. For the first phase, the adolescent was anaesthetised so that the surgeons could prepare her for the operation: they applied fixators to keep her head in the correct position and to enable them to map images previously loaded in a neuronavigator—MRI, CT, etc.—with those of the actual brain so that the surgeon had an extremely accurate guide to use during the surgery.
Once this was done, the patient was woken up and a local anaesthetic was administered so that she would be conscious during the operation but would not feel any pain. The surgeons then proceeded to excise the epileptic focus. To guarantee that they would not touch any area that would endanger the patient’s reading comprehension, they first applied a web of electrodes over her brain. Then, while a neurophysiologist stimulated the area to be operated on using a pen electrode, a neuropsychologist tested the patient to see whether there was any interference with her language and reading abilities. If there was interference, the surgeons stopped operating in that location and sought another approach.
The teenager was operated on in October 2017 and since then she has not had a single epileptic seizure.