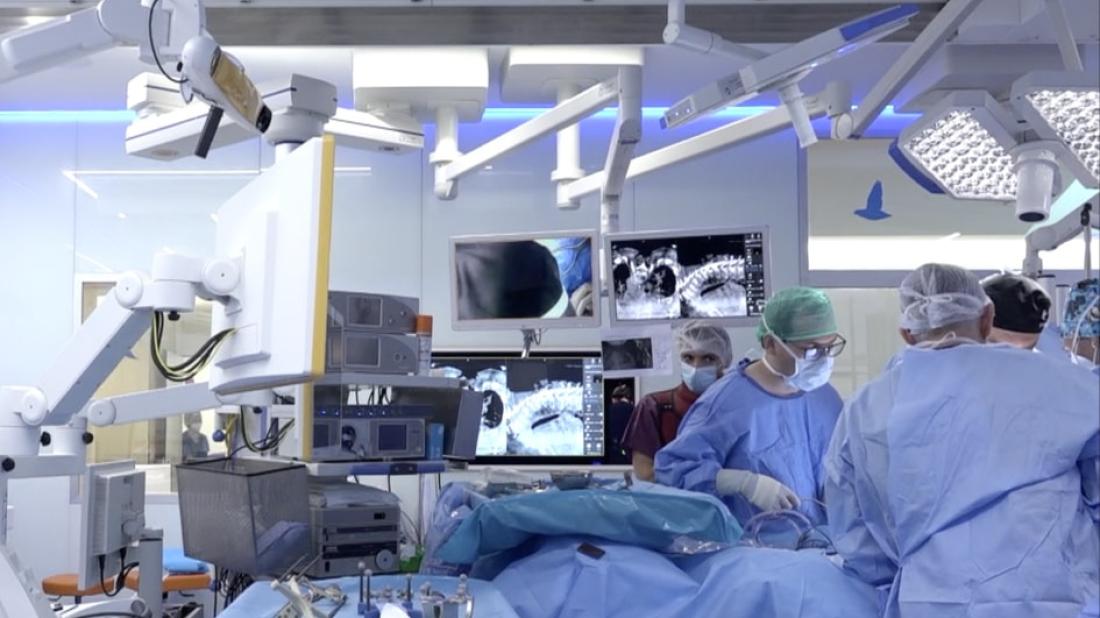
The new SJD Barcelona Children's Hospital surgical block and its hybrid operating theatre enable the use of these techniques in cases of complex spinal surgery.
The Orthopaedics and Traumatology Department is among the departments with the highest activity in the operating theatres at SJD Barcelona Children's Hospital, with a yearly average of 1,600 surgical procedures. In 2019 alone, more than a hundred surgeries for scoliosis were performed. This figure is on track to be matched in 2020, despite the repercussions of the COVID-19 pandemic for the hospital's surgical activity.
With its gradual return to activity after the pandemic and the recovery of its surgical activity, the Spinal Unit, consisting of Dr Alejandro Peiró and Dr Imma Vilalta, has performed the first spinal surgery in the hospital's hybrid operating theatre, using the Azurion imaging system (for image-guided surgery) combined with a neuronavigation system for spinal surgery. The imaging system enables 3D reconstruction of the patient's spinal anatomy. The neuronavigation system allows surgeons to monitor the progress of a surgical procedure in real time and is used as a GPS for a more precise and efficient operation.
"Combining the two techniques has enabled us to perform safer, more precise surgery on a patient with mucopolysaccharidosis and a severe spinal deformity", said Dr César Galo García Fontecha, Head of the Orthopaedics and Traumatology Department. In this case, the patient's very small vertebrae as a result of his disease, in addition to his short height for his age and uncommon anatomy, made the operation particularly complex and delicate.
This combined technique is useful in pediatric traumatology, as having a GPS enables surgeons to operate more precisely on abnormal anatomy. "The actual imaging provided by the neuronavigation system to place screws allows us to work more precisely than anatomical references do", explained Dr Peiró, a surgeon specialising in scoliosis and spinal deformities. "In the most complex cases, the neuronavigation system is safer. In surgery performed without this tool, slight hardware deviation occurs in up to 30% of cases. This technique reduces that margin of error considerably", Peiró added.
Fewer complications, better recovery and more effective surgery
The main benefit of this technology, which is not in common use in pediatric surgery in Spain, is —as mentioned— its precision. Working with the neuronavigation system allows surgeons to use tools that reduce time in surgery by 60%. Swifter surgery translates to less patient bleeding, a lower infusion rate and fewer infections. As a result, complications are substantially reduced. Furthermore, the postoperative period is less painful and pediatric patients' hospital stays are shorter.
Cutting time in surgery by more than half also allows more patients to receive care and brings costs down to an average of €8,000 per patient undergoing surgery. Increased operating theatre efficiency is important in planned spinal surgery (not just scoliosis procedures), which are ideally performed early. "Growing patients must have surgery as early as possible, because when surgery is performed early, the patient's recovery is quicker and more satisfactory in most cases", said Peiró.